
Chapter 07: IV Fluid and Parenteral Nutrition Calculations Daily fluid requirements

07
CHAPTER
IV Fluid and Parenteral Nutrition Calculations Daily fluid requirements
What Are Daily Fluid Requirements?
- Daily fluid requirements estimate the volume of water needed over 24 hours to maintainnormal hydration, electrolyte balance, and organ function, especially when a patient is unable to take oral fluids.
When Is This Clinically Useful in Pharmacy?
- Startingmaintenance IV fluids Preparing TPN (Total Parenteral Nutrition)
- Managing fluid status incritically ill or NPO patients
- Adjusting fluids in patients withrenal, liver, or heart dysfunction
Where Is It Used in Clinical Practice?
- Oninpatient medical and surgical floors
- InICU settings for fluid balance
- Duringperioperative care
- InTPN formulation and electrolyte management
Why Is It Important?
- Preventsdehydration and hypoperfusion
- Avoidsfluid overload, which can cause edema, hyponatremia, or pulmonary complications
- Supportsrenal perfusion and medication distribution
- Helps achieveelectrolyte stability
How to Calculate Daily Maintenance Fluid? Adults:
- 1500 mL + (20 mL × [weight in kg – 20]) memorize this formula (Use this formula if the patient weighs >20 kg)
Example:
AC is a 60-year-old female admitted to the hospital with gastrointestinal (GI) complications. She will be NPO (nothing by mouth) for the next 9 days. Patient weight: 65 kg, Phosphate: 3.5mg/dL, and Creatinine Clearance (CrCl): 1.4mg/dL
Calculate the patient’s daily fluid requirement.
Fluid Requirement=1500 mL+20 mL×((kg)−20)
Fluid Requirement=1500 mL+20 mL×((65)−20)= 2400mL/day
Quick estimate used 30–40 mL/kg/day for adults
Use for rapid clinical decisions
65 kg × 30 = 1950 mL
65 kg × 40 = 2600 mL
Range: 1950–2600 mL/day
Pediatric Example:
Pediatrics: 100/50/20 Rule
| Weight Range | Daily Fluid Need |
|---|---|
| First 10 kg | 100 mL/kg |
| Next 10 kg | 50 mL/kg |
| Each kg > 20 kg | 20 mL/kg |
Example:
LM is a 5-year-old male admitted with viral gastroenteritis. He has been vomiting and unable to tolerate oral intake. He is expected to remain NPO for at least 48 hours. You are asked to calculate his daily maintenance fluid requirement. Weight: 22 kg, Serum Creatinine, Electrolytes: Within normal limits Clinical Note: Mild dehydration suspected
Use the 100/50/20 Rule for Pediatric Maintenance Fluids:
| Weight Segment | Fluid Requirement |
|---|---|
| First 10 kg | 100 mL/kg × 10 = 1000 mL |
| Next 10 kg | 50 mL/kg × 10 = 500 mL |
| Remaining 2 kg | 20 mL/kg × 2 = 40 mL |
Total = 1000 + 500 + 40 = 1540 mL/day
Daily Fluid Needs – Quick Recipe Card
- Gather Patient Weight (kg)
- Convert from pounds if needed (1 kg = 2.2 lbs)
- Use the Right Formula
- Adults:1500 mL + 20 × (kg – 20)
- OR:30–35 mL/kg/day for rapid estimate
- Pediatrics:Use 100/50/20 rule
- Adjust for Clinical Conditions
- 🔻 Decrease for: CHF, renal or hepatic impairment
- 🔺 Increase for: fever, diarrhea, NG suction, burns
- Round Appropriately
- Round to the nearest 50–100 mL based on clinical context
IV infusion rates (mL/hr, gtt/min)
What Are IV Infusion Rates?
- IV infusion rates tell us how fast a medication or fluid should be delivered through an IV line. The goal is to give the right amount, at the right speed, for safety and effectiveness.
- There are two ways we express infusion rates:
- mL/hr = milliliters per hour → used with IV pumps
- gtt/min = drops per minute → used with manual gravity drip sets
- There are two ways we express infusion rates:
- When Is This Clinically Useful in Pharmacy?
- When setting up maintenance IV fluids
- When preparing electrolytes, antibiotics, or TPN
- For emergency or critical care drips
- Anytime a provider writes “infuse over X hours” and a rate is needed
- Where Is It Used in Clinical Practice?
- Hospital floors
- ICU and Emergency Rooms
- Home health or hospice IV infusions
- IV rooms when mixing sterile products
- During rounds when adjusting meds at bedside
- Why Do We Calculate This in Pharmacy?
- To make sure the nurse gives the right amount (not too fast or too slow)
- If the infusion is too fast, it can cause:
- Toxicity
- Fluid overload
- If it’s too slow, the drug might:
- Not work in time
- Drop below therapeutic levels
- When verifying hospital or home IV orders
- During emergency drips or TPN
- To protect the patient from overdosing or underdosing
- To make sure the nurse gives the right amount (not too fast or too slow)
Quick Recipe Card
| Step | What to Do | Tips / Examples |
|---|---|---|
| 1 | Identify what’s being asked | Is it mL/hr (pump) or gtt/min (manual drip)? |
| 2 | Gather the given info | – Total volume (mL) – Time (hr or min) – Drop factor (if drip) |
| 3 | Choose the correct formula | – mL/hr = Volume ÷ Time (hr) – gtt/min = (Volume × Drop factor) ÷ Time (min) |
| 4 | Convert units if needed | 1 hour = 60 minutes 1 kg = 2.2 lb (if used for dosing step before infusion) |
| 5 | Solve and round your answer | – Round gtt/min to a whole number – Round mL/hr to 1 decimal or whole number |
| 6 | Label your answer | Write mL/hr or gtt/min — don’t forget! |
| 7 | Double-check your work | Does the rate make sense? Is it too fast or too slow for the volume and time? |
Step 1: Write What the Question Is Asking For On the left side of your page or workspace, clearly write what unit you’re trying to solve for. This is your target unit.
Examples:
- Find: mcg/kg/min
- Find: mg/hr
- Find: mL/hr
Writing this down first keeps you focused and helps you build your conversion path correctly.
Step 2: Write Down All the Given Information On the right side, list all the known values from the problem. Include:
- Concentration (e.g., 4 mg in 250 mL)
- Infusion rate (e.g., 8 mL/hr)
- Patient weight (e.g., 70 kg)
- Any time values (e.g., 30 minutes)
Step 3: Cancel Units Until You Reach Your Target
Now, start solving by stacking conversions (dimensional analysis). Your goal is to cancel out all the units except the one you’re solving for.
Ask yourself:
- Do my units match?
- Am I converting time or weight?
- Am I using the correct concentration?
Work one step at a time and let the units guide you.
1) Infuse 1000 mL of normal saline (NS) over 8 hours using an IV pump.
What is the infusion rate in mL/hr?
2) Infuse 500 mL over 4 hours using a macrodrip set with a drop factor of 15 gtt/mL.
What is the drip rate in gtt/min?
3) Infuse 250 mL of ceftriaxone IV over 30 minutes. The nurse needs the rate in mL/hr for the IV pump.
What is the correct mL/hr setting?
4) A patient weighing 70 kg is prescribed propofol at a rate of 0.5 mg/kg/hr. The nurse needs to know how many mg per hour the patient should receive.
What is the correct dose in mg/hr?
5) A norepinephrine infusion is running at 8 mL/hr. The bag contains 4 mg of norepinephrine in 250 mL of D5W. The patient weighs 60 kg.
What is the infusion rate in mcg/kg/hr?
TPN macronutrient calorie calculations
What is TPN and What Does It Contain?
Total Parenteral Nutrition (TPN) is a method of providing complete nutrition through the veins when a patient cannot eat or use their GI tract.
TPN contains macronutrients that supply calories:
| Macronutrient | Function | Provides Calories |
|---|---|---|
| Dextrose | Main energy source (carbohydrate) | 3.4 kcal/g |
| Amino Acids | Build and repair tissues (protein source) | 4 kcal/g |
| IV Lipids (10%) | Energy + essential fatty acids | 1.1 kcal/mL (~11 kcal/g) |
| IV Lipids (20% or higher) | Energy + essential fatty acids | 2 kcal/mL (~10 kcal/g) |
Who Needs TPN?
TPN is given to patients who cannot eat, digest, or absorb nutrients by mouth or tube.
Common patients include:
- Critically ill in ICU
- Short bowel syndrome
- Post-surgical patients with ileus or obstruction
- Severe Crohn’s disease or pancreatitis
- Cancer patients undergoing chemotherapy
When is TPN used?
- When enteral nutrition (tube feeds) is not possible or contraindicated.
- If the patient is expected to be NPO (nothing by mouth) for >5–7 days.
- Used short-term in hospital or long-term at home (Home TPN).
Where is TPN Administered?
- TPN is given intravenously through:
- A central venous catheter (preferred for high dextrose concentrations)
- A peripherally inserted central catheter (PICC line)
- Infused over 24 hours (continuous) or sometimes cyclically (overnight).
- TPN is given intravenously through:
Why is Calorie Calculation Important?
Because each macronutrient contributes differently to total calories, accurate calculation is vital to:
- Prevent underfeeding or overfeeding
- Meet daily energy needs
- Avoid complications like hyperglycemia, fatty liver, or excess CO₂ production
How to Calculate TPN Calories
How to Calculate TPN Calories
Calculating Total Parenteral Nutrition (TPN) calories involves adding up the calories from each macronutrient in the formulation: dextrose, amino acids (protein), and lipids (fats).
Here’s the step-by-step method:
Calories from Dextrose
- Dextrose in TPN provides 3.4 kcal per gram (not 4 kcal like in enteral nutrition).
- Formula:
Calories from Dextrose = grams of dextrose × 3.
Example:
If dextrose = 200 g
200 × 3.4 = 680 kcal
Calories from Amino Acids (Protein)
- Amino acids provide 4 kcal per gram.
- Formula:
Calories from Amino Acids = grams of amino acids × 4
- Example:
If amino acids = 75 g
- Example:
75 × 4 = 300 kcal
Calories from Lipids (Fat)
- Lipid emulsions have different caloric values based on concentration:
- 10% lipid → 1.1 kcal/mL
- 20% lipid → 2 kcal/mL
- 30% lipid → 3 kcal/mL
- Formula:
- Lipid emulsions have different caloric values based on concentration:
Calories from Lipids = volume (mL) × kcal/mL
- Example:
If 20% lipid = 250 mL
- Example:
250 × 2 = 500 kcal
Total Calories
- Formula:
Total Calories = Dextrose kcal + Amino Acid kcal + Lipid kcal kcal
- Example:
From above:
- Example:
680 + 300 + 500 = 1,480 kcal total
Quick Reference Table:
Dextrose 3.4 kcal/g
Amino acids 4 kcal/g
10% Lipid 1.1 kcal/mL
20% Lipid 2 kcal/mL
30% Lipid 3 kcal/mL
QUICK EXAMPLE
Prescription:
- Dextrose 20%, 1500 mL
- Amino acids 5%, 1000 mL
- Lipid 20%, 250 mL
Calculation:
Dextrose:
- 300 g ×3.4 kcal/g =1020 kcal
Amino acids:
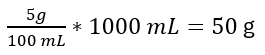
- 50×4 kcal/g =200 kcal
Lipids:
250×2 kcal/mL = 500 kcal or by step by step:
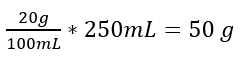
- 50 g * 10 kcal/g = 500 kcal
Total:
1020+200+500=1720 kcal

